Credit CDC
Update: Transcript | Audio now available for the CDC’s Monday Afternoon press conference.
# 9257
If there is anything good that can be said to be coming out of the Ebola epidemic, it is that it is forcing us to take a hard look at our emergency response and pandemic preparedness plans – and to work out the kinks – before we find ourselves blindsided by a more rapidly moving and highly virulent pandemic.
CDC interim guidance on Ebola continues to evolve as more is learned about dealing with the virus in modern healthcare settings and in a highly mobile developed nation, and it is not unreasonable to assume that over time that guidance may change further.
Last week the CDC announced a program of Active Post-Arrival Monitoring for Travelers from Impacted Countries, which provided arrivals from Ebola affected countries with a CARE (Check & Report Ebola) Kit and instructions on taking their temperature, and maintaining contact with local health department officials.
While introducing a higher degree of monitoring, it relied upon the traveler to self-check and to report symptoms on a daily basis during the 21 day incubation period, and imposed no real restrictions on movement or travel.
Two days later New York City detected their first imported Ebola case – and the newspapers had a field day analyzing that person’s movements around the city prior to calling in that he was ill. As a result, the Governors of New York and New Jersey announced their own, more restrictive quarantine protocols, which have sparked heated debate.
Today, CDC Director Thomas Frieden held a press conference to announce new, tighter CDC guidelines – that while less restrictive than some of the state plans rolled out over the weekend – he believes are appropriate and not overly onerous.
Whether individual states will adopt them – or continue to go their own way – is something we will have to wait to see.
Today’s guidance also includes guidance on monitoring and movement control protocols for people who may have been exposed (i.e. Healthcare workers, family members, etc.) to an Ebola case in this country. For the purposes of triage, potentially exposed people are divided into 4 risk groups:
- High Risk
- Some Risk
- Low Risk (but not zero)
- No Risk
Full details on how each risk group would be treated can be viewed at the link below:
Monitoring Symptoms and Controlling Movement to Stop Spread of Ebola
For Immediate Release: Monday, October 27, 2014
Contact: Media Relations, Office of Communication
(404) 639-3286
Fact SheetPurpose
This fact sheet explains CDC’s updated guidance to protect America from Ebola. This updated guidance focuses on strengthening how we monitor people who may have been exposed to Ebola and how medical professionals will oversee their care and, when warranted to protect the public health or our communities, limit their movement or activities. Through these changes, CDC and state and local health departments seek to support people who may have been exposed to Ebola, while also continuing to stop Ebola at its source in West Africa through the valor of our health care workers who serve. These changes will help ensure their symptoms are monitored and a system is in place to quickly recognize when they need to be routed to care. These actions will better protect potentially exposed individuals and the American public as a whole.
Key changes to the movement and monitoring guidance
- New risk levels are given for people who may have been exposed to Ebola, as well as for those not at risk for the disease.
- The guidance recommends stricter actions for escalating level of risk based on the type of exposure.
- State and local public health authorities are advised to use active monitoring or direct active monitoring rather than having people monitor themselves.
- Specific guidance is given about monitoring health care workers who cared for patients with Ebola in a country with widespread transmission, and people who visited an Ebola Treatment Unit in one of those countries.
- Specific guidance is also given about monitoring health care workers who provided care of patients with Ebola in the United States
New risk levels
The new guidance defines four risk levels based on degree of exposure:
High risk—direct contact of infected body fluids through:
- needle stick, or splashes to eyes, nose, or mouth
- getting body fluids directly on skin
- handling body fluids, such as in a laboratory, without wearing personal protective equipment (PPE) or following recommended safety precautions
- touching a dead body without correctly wearing PPE in a country with widespread Ebola transmission
- living with and caring for a person showing symptoms of Ebola
Some risk—
- close contact with a person showing symptoms of Ebola such as in a household, health care facility, or the community (no PPE worn). Close contact means being within 3 feet of the person with Ebola for a long time without wearing PPE.
- in countries with widespread Ebola transmission: direct contact with a person showing symptoms of Ebola while wearing PPE
Low risk (but not zero)—
- having been in a country with widespread Ebola transmission within the previous 21 days and having no known exposure
- being in the same room for a brief period of time (without direct contact) with a person showing symptoms of Ebola
- having brief skin contact with a person showing symptoms of Ebola when the person was believed to be not very contagious
- in countries without widespread Ebola transmission: direct contact with a person showing symptoms of Ebola while wearing PPE
- travel on an airplane with a person showing symptoms of Ebola
No risk—
- contact with a person who is NOT showing symptoms AFTER that person was in contact with a person with Ebola
- contact with a person with Ebola BEFORE the person was showing symptoms
- having traveled to a country with Ebola outbreak MORE than 21 days ago
- having been in to a country where there is no widespread Ebola transmission (e.g., the United States), and having no other exposures to Ebola
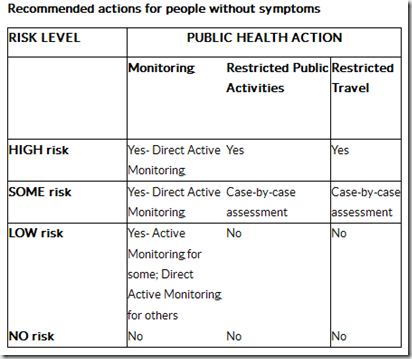
Public health officials will use these risk levels along with assessing symptoms to decide how best to monitor for symptoms and what other restrictions may be needed. The table on the following page provides further information about CDC’s recommended action for each risk level.