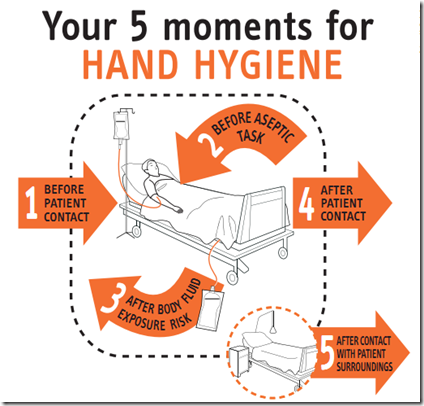
Credit WHO
#14,316
I confess to carrying a little bottle of hand sanitizer in my car year-round, and usually slip it into my pocket for more frequent access during `flu season'.
While I can't prove its effectiveness - between getting a flu shot every year and using copious amounts of sanitizer - I haven't suffered a respiratory infection in the past 10 years.We've a new study, however - published yesterday in ASM Journal mSphere - that questions the effectiveness of ordinary hand sanitizer against flu germs . . . at least in certain patient care settings.
This isn't the first time we've seen the limitations of these alcohol-based hand sanitizers, particularly when dealing with norovirus and C.diff (see CDC C. Diff FAQ & CMAJ: Hand Sanitizers May Be `Suboptimal’ For Preventing Norovirus).Today's study investigates the effect of mucus in protecting the virus from ethanol based disinfectants (EBDs). While 30 seconds of rubbing hand sanitizer kills dried flu germs on the hands, it takes between 2 and 4 minutes of EBD rubbing to kill wet `protected' flu viruses.
Thirty seconds of soap and water handwashing, however, killed both wet and dried flu viruses.While not a panacea for infection control, EBDs are likely still effective against flu virus contaminated surfaces (fomites); door knobs, cell phones, shopping cart handles, and a myriad of other hard surfaces.
So I'll not be giving up my EBD hand sanitizing ways when I'm out in public.First the press release from ASM, followed by a link to and excerpts from the study.
The abstract to the full study (which is open-access) follows:
Towards Better Hand Hygiene for Flu Prevention
Sept. 18, 2019
Washington, DC – September 18, 2019 – Rubbing hands with ethanol-based sanitizers should provide a formidable defense against infection from flu viruses, which can thrive and spread in saliva and mucus. But findings published this week in mSphere challenge that notion — and suggest that there’s room for improvement in this approach to hand hygiene.
The influenza A virus (IAV) remains infectious in wet mucus from infected patients, even after being exposed to an ethanol-based disinfectant (EBD) for two full minutes, report researchers at Kyoto Profectural University of Medicine, in Japan. Fully deactivating the virus, they found, required nearly four minutes of exposure to the EBD.
The secret to the viral survival was the thick consistency of sputum, the researchers found. The substance’s thick hydrogel structure kept the ethanol from reaching and deactivating the IAV.
“The physical properties of mucus protect the virus from inactivation,” said physician and molecular gastroenterologist Ryohei Hirose, Ph.D, MD., who led the study with Takaaki Nakaya, PhD, an infectious disease researcher at the same school. “Until the mucus has completely dried, infectious IAV can remain on the hands and fingers, even after appropriate antiseptic hand rubbing.”
The study suggests that a splash of hand sanitizer, quickly applied, isn’t sufficient to stop IAV. Health care providers should be particularly cautious: If they don’t adequately inactivate the virus between patients, they could enable its spread, Hirose said.
The researchers first studied the physical properties of mucus and found — as they predicted — that ethanol spreads more slowly through the viscous substance than it does through saline. Then, in a clinical component, they analyzed sputum that had been collected from IAV-infected patients and dabbed on human fingers. (The goal, said Hirose, was to simulate situations in which medical staff could transmit the virus.) After two minutes of exposure to EBD, the IAV virus remained active in the mucus on the fingertips. By four minutes, however, the virus had been deactivated.
Previous studies have suggested that ethanol-based disinfectants, or EBDs, are effective against IAV. The new work challenges those conclusions. Hirose suspects he knows why: Most studies on EBDs test the disinfectants on mucus that has already dried. When he and his colleagues repeated their experiments using fully dried mucus, they found that hand rubbing inactivated the virus within 30 seconds. In addition, the fingertip test used by Hirose and his colleagues may not exactly replicate the effects of hand rubbing, which through convection might be more effective at spreading the EBD.
For flu prevention, both the Centers for Disease Control and Prevention and the World Health Organization recommend hand hygiene practices that include using EBDs for 15-30 seconds. That's not enough rubbing to prevent IAV transmission, said Hirose.
The study wasn't all bad news: The researchers did identify a hand hygiene strategy that works, also sanctioned by the WHO and CDC. It's simple: Wash hands, don't just rub them. Washing hands with an antiseptic soap, they found, deactivated the virus within 30 seconds, regardless of whether the mucus remained wet or had dried.
Situations Leading to Reduced Effectiveness of Current Hand Hygiene against Infectious Mucus from Influenza Virus-Infected Patients
Ryohei Hirose, Takaaki Nakaya, Yuji Naito, Tomo Daidoji, Risa Bandou, Ken Inoue, Osamu Dohi, Naohisa Yoshida, Hideyuki Konishi, Yoshito Itoh
Helene F. Rosenberg, Editor
DOI: 10.1128/mSphere.00474-19
ABSTRACT
Both antiseptic hand rubbing (AHR) using ethanol-based disinfectants (EBDs) and antiseptic hand washing (AHW) are important means of infection control to prevent seasonal influenza A virus (IAV) outbreaks. However, previous reports suggest a reduced efficacy of ethanol disinfection against pathogens in mucus. We aimed to elucidate the situations and mechanisms underlying the reduced efficacy of EBDs against IAV in infectious mucus. We evaluated IAV inactivation and ethanol concentration change using IAV-infected patients’ mucus (sputum). Additionally, AHR and AHW effectiveness against infectious mucus adhering to the hands and fingers was evaluated in 10 volunteers.
Our clinical study showed that EBD effectiveness against IAV in mucus was extremely reduced compared to IAV in saline. IAV in mucus remained active despite 120 s of AHR; however, IAV in saline was completely inactivated within 30 s. Due to the low rate of diffusion/convection because of the physical properties of mucus as a hydrogel, the time required for the ethanol concentration to reach an IAV inactivation level and thus for EBDs to completely inactivate IAV was approximately eight times longer in mucus than in saline.
On the other hand, AHR inactivated IAV in mucus within 30 s when the mucus dried completely because the hydrogel characteristics were lost. Additionally, AHW rapidly inactivated IAV. Until infectious mucus has completely dried, infectious IAV can remain on the hands and fingers, even after appropriate AHR using EBD, thereby increasing the risk of IAV transmission. We clarified the ineffectiveness of EBD use against IAV in infectious mucus.
IMPORTANCE Antiseptic hand rubbing (AHR) and antiseptic hand washing (AHW) are important to prevent the spread of influenza A virus (IAV). This study elucidated the situations/mechanisms underlying the reduced efficacy of AHR against infectious mucus derived from IAV-infected individuals and indicated the weaknesses of the current hand hygiene regimens.
Due to the low rate of diffusion/convection because of the physical properties of mucus as a hydrogel, the efficacy of AHR using ethanol-based disinfectant against mucus is greatly reduced until infectious mucus adhering to the hands/fingers has completely dried. If there is insufficient time before treating the next patient (i.e., if the infectious mucus is not completely dry), medical staff should be aware that effectiveness of AHR is reduced. Since AHW is effective against both dry and nondry infectious mucus, AHW should be adopted to compensate for these weaknesses of AHR.