"In the US, six in ten adults have one or more chronic health conditions, including heart disease, lung disease, and diabetes, that put them at increased risk for flu and COVID-19." - NFID
#15,509
While influenza activity globally has been greatly suppressed since the emergence of COVID-19 last spring (see WHO Flu Report ) - and there remains a good deal of uncertainty over the timing and magnitude of its return in the Northern Hemisphere this winter - concerns over influenza's interaction with the coronavirus pandemic are not unwarranted.
Not only would as `twindemic' greatly increase the burden on the healthcare delivery system, we've seen recent studies suggesting that coinfection with Influenza A and COVID-19 can greatly increase the risk of death or serious illness.
PrePrint: Sequential Infection with Influenza A virus Followed by SARS-CoV-2 (In a Mouse Model)
PHE Study: Co-Infection With COVID-19 & Seasonal Influenza
While Influenza and COVID-19 can be deadly even in healthy young people, the risks go up exponentially in older individuals, particularly those with chronic health problems. And in the United States, 6 out of 10 adults have one or more chronic health conditions.
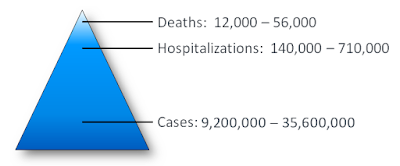
As the chart below illustrates, both COVID and Influenza tend to hospitalize individuals with chronic or underlying health conditions. This includes pregnancy (see MMWR: Two New Reports On Pregnancy & COVID-19).
In an average year, seasonal flu kills roughly as many Americans as does gun violence, or car accidents. In a bad year - such as we saw in 2017-2018, influenza can kill as many as both of those combined.
With already more than 5 times the number of deaths from COVID since last March as is normally reported in a severe flu season, the prospects of having both viruses circulating this winter is a daunting one.
Late last week NFID - the National Foundation for Infectious Diseases, a non-profit organization founded in 1973 - released a 20-page PDF call to action for this winter's flu season, urging increased flu vaccine uptake; particularly for those with chronic or underlying conditions.
New Call to Action Highlights Dual Threat of Influenza and COVID-19 for US Adults with Chronic Health ConditionsWashington, DC (October 15, 2020) — The National Foundation for Infectious Diseases (NFID) issued a new Call to Action report detailing the risks of co-infection with influenza (flu) and COVID-19 in adults with chronic health conditions, and the importance of flu vaccination during the 2020–2021 season. The goals of the report, The Dangers of Influenza and COVID-19 in Adults with Chronic Health Conditions, have been supported by more than 35 leading medical organizations, including the American College of Cardiology, American College of Emergency Physicians, American Diabetes Association, and American Lung Association, who are now urging their stakeholders to prioritize flu vaccination for these high-risk populations.
In the US, six in ten adults have one or more chronic health conditions, including heart disease, lung disease, and diabetes, that put them at increased risk for flu and COVID-19. For this population, related complications include the potential exacerbation of underlying health condition(s), as a result of flu-related inflammation that may persist long after the acute infection, as well as increased risk of long-term complications, such as heart attack and stroke, after experiencing acute flu or COVID-19 infection.According to the Centers for Disease Control and Prevention (CDC), annual flu vaccination has been proven to mitigate serious flu-related complications, preventing an estimated 7.5 million flu illnesses, 3.7 million flu-associated medical visits, 105,000 flu hospitalizations, and 6,300 flu deaths in 2019–2020 alone. Yet, a recent NFID survey found that nearly one in four US adults at high risk for flu-related complications said they did not intend to get vaccinated during the 2019-2020 flu season.“Amidst the COVID-19 pandemic, patients with chronic health conditions are facing not one, but two viruses that pose a serious threat to their health and independence,” said NFID Medical Director William Schaffner, MD. “While we currently don’t have an approved COVID-19 vaccine in the US, we know that annual flu vaccination can help protect these patients from hospitalization, progressive disability, and even death. It is imperative that healthcare professionals educate patients with chronic health conditions about their risks and implement strategies to increase flu vaccination rates during the COVID-19 pandemic.”In advance of an unprecedented 2020-2021 flu season, NFID convened a multidisciplinary virtual roundtable with leading experts to explore the risks of co-circulation and co-infection with flu and SARS-CoV-2 (the virus that causes COVID-19) in adults with chronic health conditions. The resulting NFID Call to Action, which summarizes the roundtable discussions, includes best practices for administering flu vaccines in conjunction with COVID-19 mitigation efforts. Despite the limited data currently available on outcomes from co-infection with the two viruses, insights from the roundtable highlighted that the impact on patients and the US public health system could be catastrophic.“It won’t take a ‘bad’ flu season—just ‘a’ flu season to make things more difficult in the ER and elsewhere in the US healthcare system,” said Nicholas F. Vasquez, MD, vice chair of the Diversity, Inclusion, and Health Equity Section of the American College of Emergency Physicians. “Further strain due to the co-circulation of flu and COVID-19 could disrupt routine care and have detrimental consequences for adults with chronic health conditions.”The relationship between flu and heart disease is of particular concern during the current pandemic, as severe COVID-19 outcomes have also been associated with pre-existing cardiovascular conditions and post-infection injury to heart tissue. Over the past eight US flu seasons, nearly 47 percent of patients hospitalized for flu had heart disease, making it the most common underlying health condition associated with flu-related complications. Fortunately, flu vaccination can serve as an effective prevention strategy in these patients. One study estimated the flu vaccine is between 15 to 45 percent effective in preventing heart attacks and strokes, making it equal to or more effective than smoking cessation, statins, and antihypertensive therapy.“I am greatly concerned for heart disease patients this flu season. It is already well-documented that heart disease is a risk factor for severe flu-related illness, but with COVID-19, we are entering a dangerous and uncharted territory,” said William B. Borden, MD, professor of medicine and health policy at George Washington University, representing the American College of Cardiology. “The most important thing we can do to protect these patients is to ensure they are getting their annual flu vaccine. I am making it a point this season to strongly recommend a flu vaccine to every heart patient I see and urge my colleagues to do the same.”To help increase flu vaccination rates, the NFID Call to Action offers strategies and tactics for healthcare professionals, particularly specialists treating adults with chronic conditions during the 2020-2021 flu season, including communication methods for discussions with both patients and office staff, vaccine implementation strategies specific to the COVID-19 pandemic, and techniques for addressing vaccine misinformation.“All healthcare professionals, including specialty care providers, have a duty to understand the risks our patients face and advocate for any preventive measure that can preserve health and save lives,” said NFID President Patricia N. Whitley-Williams, MD, also representing the National Medical Association. “If you treat a patient with heart disease, lung disease, diabetes, or another chronic health condition, then you have a responsibility to insist upon annual flu vaccination.”Additional resources on flu and COVID-19, and the impact on adults with chronic health conditions, are available at www.nfid.org/loweryourflurisk.Sanofi Pasteur provided funding for this activity. NFID policies restrict funders from controlling program content.
There are a lot of ways to rationalize not getting the flu shot this fall, if that is what you are looking to do.
But getting the flu vaccine is one of the few proactive things you can do to lower the risks to yourself, and the people you come in contact with, of serious respiratory illness this winter. Even when it doesn't prevent infection, there is evidence (see study) suggesting the flu vaccine may reduce the severity of one's illness.
While I recognize the limitations of the flu vaccine, and consider it just one part of a layered strategy of protection (along with face covers, hand hygiene, social distancing, etc.) during this pandemic, it has the advantage of being a `get it and forget it' intervention.
And much like the flu vaccine, there is evidence that suggests getting the pneumonia vaccine may reduce death and serious illness (see The Conversation: Until a Coronavirus Vaccine Is Ready, Pneumonia Vaccines May Reduce Deaths From COVID-19) from the pandemic virus.
None of these interventions is expected to be a panacea for our COVID pandemic, but when adopted by enough people, it may make the next few months more manageable.