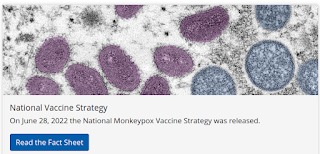
Credit CDC
#16,852
While Monkeypox isn't expected to present a society-wide epidemic threat like COVID or pandemic flu, without a coordinated national and international response, it still has the ability to spread potentially serious illness and become firmly entrenched in humans with unpredictable results.
Yesterday the CDC announced 60 new cases (n=306), while internationally the number now exceeds 3,000. Both numbers are thought to be significantly under-counted, and are expected to continue to rise as testing increases.
Later today the CDC will hold a COCA Call for clinicians on clinical diagnosis, treatment, and reporting of cases, while yesterday the CDC activated their EOC (Emergency Operations Center).
CDC Activates Emergency Operations Center for Monkeypox Response
Media Statement
For Immediate Release: Tuesday, June 28, 2022
Contact: Media Relations
(404) 639-3286
Today, CDC continues to lean forward with an aggressive public health response to the monkeypox outbreak by activating its Emergency Operations Center (EOC). This action stands up the CDC’s command center for monitoring and coordinating the emergency response to monkeypox and mobilizing additional CDC personnel and resources. CDC’s activation of the EOC allows the agency to further increase operational support for the response to meet the outbreak’s evolving challenges. It is home to more than 300 CDC staff working in collaboration with local, national, and international response partners on public health challenges. The activation of the EOC will serve to further supplement the ongoing work of CDC staff to respond to this outbreak.
Globally, early data suggest that gay, bisexual, and other men who have sex with men make up a high number of monkeypox cases. CDC continues to provide guidance and raise awareness among frontline healthcare providers and public health. CDC is also raising awareness of the current situation with the public through its website and social media in addition to direct partner and community outreach.
In June, CDC updated and expanded the monkeypox case definition and continues to encourage health care providers to consider testing for all rashes with clinical suspicion for monkeypox. Health care providers who see a patient with a rash that resembles monkeypox or might be more characteristic of more common infections (e.g., varicella zoster, herpes zoster, or syphilis) should carefully evaluate the patient for monkeypox and should consider testing. Anyone who has risk factors for monkeypox, and a new rash should seek care and testing.
Last week, CDC began shipping orthopoxvirus tests to five commercial laboratory companies, including the nation’s largest reference laboratories, to quickly increase monkeypox testing capacity and access in every community. This development will facilitate increased testing, leverage established relationships between clinics, hospitals and commercial laboratories, and support our ability to better understand the scope of the current monkeypox outbreak.
Please visit the CDC website, which is updated daily, for the latest information related to our response.
Late yesterday the HHS and White House held a press call where they unveiled the HHS's plan to acquire, and distribute, over 1.6 million doses of Monkeypox (JYNNEOS) vaccine over the coming months, and to expand the nation's testing capacity.
This vaccination plan is targeted at the highest risk individuals, and those who may have been exposed, and since it requires 2-shots, will be enough for about 800,000 individuals.
The HHS press release follows, after which I'll have a bit more about the JYNNEOS vaccine.
HHS Announces Enhanced Strategy to Vaccinate and Protect At-Risk Individuals from the Current Monkeypox Outbreak
The U.S. Department of Health and Human Services (HHS) today announced an enhanced nationwide vaccination strategy to mitigate the spread of monkeypox. The strategy will vaccinate and protect those at-risk of monkeypox, prioritize vaccines for areas with the highest numbers of cases, and provide guidance to state, territorial, tribal, and local health officials to aide their planning and response efforts.
Under the strategy, HHS is rapidly expanding access to hundreds of thousands of doses of the JYNNEOS vaccine for prophylactic use against monkeypox in areas with the highest transmission and need, using a tiered allocation system. Jurisdictions can also request shipments of the ACAM2000 vaccine, which is in much greater supply, but due to significant side effects is not recommended for everyone.
“Within days of the first confirmed case of monkeypox in the United States, we quickly began deploying vaccines and treatment to help protect the American public and limit the spread of the virus,” said HHS Secretary Xavier Becerra. “While monkeypox poses minimal risk to most Americans, we are doing everything we can to offer vaccines to those at high-risk of contracting the virus. This new strategy allows us to maximize the supply of currently available vaccines and reach those who are most vulnerable to the current outbreak.”
HHS will provide 296,000 doses of JYNNEOS vaccine. Of that amount, 56,000 doses will be made available immediately, and an additional 240,000 doses will be made available in the coming weeks. HHS expects more than 750,000 additional JYNNEOS doses to be made available over the summer, and an additional 500,000 doses will undergo completion, inspection, and release throughout the fall, totaling 1.6 million doses available this year.
JYNNEOS vaccine will be allocated using a four-tier distribution strategy that prioritizes jurisdictions with the highest case rates of monkeypox. Within each tier, doses of JYNNEOS will be allocated based on the number of individuals at risk for monkeypox who also have pre-existing conditions, like HIV.
The Advisory Committee on Immunization Practices currently recommends vaccination for those at high risk following a confirmed monkeypox exposure. Given the large number of contacts and difficulty in identifying all contacts during the current outbreak, vaccine will now be provided to individuals with confirmed and presumed monkeypox exposures. This includes those who had close physical contact with someone diagnosed with monkeypox, those who know their sexual partner was diagnosed with monkeypox, and men who have sex with men who have recently had multiple sex partners in a venue where there was known to be monkeypox or in an area where monkeypox is spreading.
“We are focused on making sure the public and health care providers are aware of the risks posed by monkeypox and that there are steps they can take –through seeking testing, vaccines and treatments – to stay healthy and stop the spread,” said Centers for Disease Control and Prevention (CDC) Director Rochelle Walensky, M.D., M.P.H.
To date, the HHS Office of the Assistant Secretary for Preparedness and Response (ASPR), in coordination with the CDC, has responded to requests from 32 jurisdictions, deploying more than 9,000 doses of vaccine and 300 courses of antiviral treatments. HHS will continue to evolve and strengthen its vaccine supply and distribution strategy to ensure the communities most in need have access to vaccinations to combat monkeypox. This includes being in regular communication with states and jurisdiction to monitor case rates and be responsive to requests made by jurisdiction to ensure the vaccine strategy continues to meet needs in real-time.
Today’s expanded vaccine strategy is part of the Biden-Harris Administration’s broader monkeypox outbreak response plan to mitigate the spread of the virus and protect those at highest risk. From day one of the outbreak, the Biden Administration acted with urgency to deploy testing and treatments to communities most impacted, scaling testing capacity to more than 70 labs in 48 states and began shipping its FDA-cleared orthopoxvirus tests last week to five major commercial labs to further increase testing capacity and convenience in every community. The Administration is also communicating regularly with community leaders, health care providers, and stakeholders in high-risk communities to raise awareness of the outbreak, and increase access to tests, vaccines, and treatments.
“We have vaccines and treatments to respond to the current monkeypox outbreak thanks to years of sustained investment and planning,” said HHS Assistant Secretary for Preparedness and Response Dawn O’Connell. “Our goal right now is to ensure that the limited supply of JYNNEOS vaccine is deployed to those who can benefit from it most immediately, as we continue to secure additional vaccine doses.”
In 2019, FDA licensed JYNNEOS, a replication-deficient MVA vaccine, for prevention of smallpox or monkeypox disease in adults aged ≥18 years determined to be at high risk for infection with these viruses. JYNNEOS is administered by subcutaneous injection as a 2-dose series delivered 28 days apart. There is no major cutaneous reaction, also known as a “take” (a vaccine site lesion often used as a marker of successful vaccination with replication-competent vaccines such as ACAM2000), following vaccination with JYNNEOS and consequently no risk for inadvertent inoculation or autoinoculation. The effectiveness of JYNNEOS was inferred from the immunogenicity of JYNNEOS in clinical studies and from efficacy data from animal challenge studies.
The older ACAM2000 smallpox vaccine is still available, but is a live-virus vaccine, and carries a higher risk of adverse side effects and cannot be given to everyone.