#18,066
A dozen years ago the CDC developed the IRAT (Influenza Risk Assessment Tool) to evaluate the risks of novel flu viruses with zoonotic potential. In 2012, the list was pretty short:But 2013-2014 was a major turning point in the evolution of avian (and to a lesser extent, other) flu viruses. H7N9 appeared in China, along with H5N6, H10N8, H9N2 G1, along with several swine & canine viruses.
By the end of 2016, the number of viruses on the list had tripled (n=12).
Can the IRAT predict a future pandemic?
No. The IRAT is an evaluative tool, not a predictive tool. Flu is unpredictable, as are future pandemics.But the IRAT can help planners decide which viruses pose the greatest risks, so they can prioritize their efforts and investments. Today, there are 24 novel influenza A viruses on the IRAT list, with the most recent addition (July 2023) being the 2022 mink-derived H5N1 virus from Spain.
While that assessment increased a number of its risk factors over earlier H5N1 viruses, a few days ago - in Nature Dispatch: Risk Assessment On HPAI H5N1 From Mink - we saw new evidence of limited airborne transmission via ferrets, which may require additional scrutiny.
Of the 24 novel flu viruses on the CDC's IRAT list, 9 are H5 viruses (4 H5N1, 2 H5N8, 2 H5N6, and 1 H5N2), far and away the most represented HA type. H7 viruses (H7N9, H7N7, H7N8) come in second, appearing 6 times.
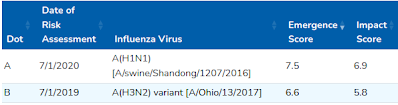
But in terms of likelihood of emergence, two swine viruses currently top the list:
Beginning the process of conducting a pandemic risk assessment on the virus from the human infection in Texas (A/Texas/37/2024) using the Influenza Risk Assessment Tool (IRAT). The IRAT is an evaluation tool developed by CDC and external flu experts that assesses the potential pandemic risk posed by novel influenza A viruses. The IRAT uses 10 risk elements to measure the potential of an influenza virus to emerge to cause a pandemic as well as the potential public health impact that a pandemic caused by that virus would have.
An IRAT is a multi-step process that can take months to complete. (More on IRAT below.) The current assessment of the risk level to the general public, which is based on available epidemiologic and laboratory data, remains low.
CDC A(H5N1) Bird Flu Response Update May 17, 2024
(excerpts)
May 17, 2024 – CDC continues to respond to the public health challenge posed by a multistate outbreak of avian influenza A(H5N1) virus, or “A(H5N1) virus,” in dairy cows and other animals in the United States. CDC is working in collaboration with the U.S. Department of Agriculture (USDA), the Food and Drug Administration (FDA), state public health and animal health officials, and other partners using a One Health approach. USDA is now reporting that 51 dairy cattle herds in nine U.S. states have confirmed cases of A(H5N1) virus infections in cattle. There have been no additional human cases detected since the one recent case from Texas was reported on April 1, 2024. [1][2]
Among other activities previously reported in past spotlights and still ongoing, recent highlights of CDC’s response to this outbreak of influenza A(H5N1) virus in dairy cattle and other animals include:
(Snip)
- Continuing to support states that are monitoring people with exposure to cows, birds, or other domestic or wild animals infected, or potentially infected, with avian influenza A(H5N1) viruses. To date, more than 300 people have been monitored as a result of their exposure to infected or potentially infected animals, and at least 37 people who have developed flu-like symptoms have been tested as part of this targeted, situation-specific testing. All except the one case in Texas have tested negative. Testing of exposed people who develop symptoms is at the state or local level, and CDC conducts confirmatory testing as needed.
- Working on a plan for enhanced, nationwide summer monitoring to help ensure that even rare cases of A(H5N1) virus infection in the community would be detected. This plan includes increasing the number of influenza virus specimens that are tested and then subtyped in public health laboratories, which can detect A(H5N1). Nationally, since March 24, 2024, almost 11,000 specimens have been tested for influenza in public health laboratories as part of this surveillance stream. While influenza testing typically declines over the summer, this approach would maintain an increased level of testing. More information on this will be forthcoming.
- Continuing to monitor flu surveillance data, especially in areas where A(H5N1) viruses have been detected in dairy cattle or other animals, for any unusual trends including in flu-like illness, conjunctivitis, or influenza virus activity.
- CDC posted influenza A wastewater surveillance data for this first time this week. Wastewater surveillance complements other existing human flu surveillance systems to monitor trends in influenza viruses. Current wastewater monitoring methods detect influenza A viruses but do not distinguish the subtype or source of the influenza A virus (whether it is from humans or animals). Reported levels of influenza A virus from each site are compared against levels reported by the same site during the prior flu season. When influenza A levels in wastewater are high (at the 80th percentile or higher), that triggers follow up by CDC, including outreach to the relevant jurisdiction to determine the source of the signal and intensive surveillance review. The data are presented in the format of an interactive map and updated weekly.
- Overall, for the most recent week of data, CDC flu surveillance systems show no indicators of unusual flu activity in people, including avian influenza A(H5N1) viruses.
CDC RecommendationsIn addition to limiting interactions between infected animals and people, containing the outbreak among animals also is important, which underscores the urgency of the work being done by USDA and animal health and industry partners.
- People should avoid close, long, or unprotected exposures to sick or dead animals, including wild birds, poultry, other domesticated birds, and other wild or domesticated animals (including cows).
- People should also avoid unprotected exposures to animal poop, bedding (litter), unpasteurized (“raw)” milk, or materials that have been touched by, or close to, birds or other animals with suspected or confirmed A(H5N1) virus.
- CDC has interim recommendations for prevention, monitoring, and public health investigations of A(H5N1) virus infections in people. CDC also has updated recommendations for worker protection and use of personal protective equipment (PPE). Following these recommendations is central to reducing a person’s risk and containing the overall public health risk.
Trying to predict what a flu virus will - or won't - do, is a mug's game.
There is still time to correct that.
But the clock is ticking . . .