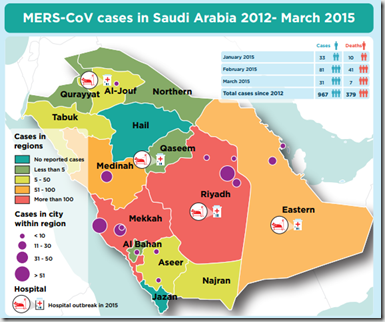
Credit WHO EMRO MERS Summary
# 9881
Even though avian flu has captured much of our attention this winter, running a close second is the MERS coronavirus, which continues to plague inhabitants of the Arabian peninsula – particularly in central and Western Saudi Arabia.
Now nearly three years into this outbreak, we still have many unanswered questions regarding its source, and how it is spreading among humans.
After seeing low levels of cases in 2012 and 2013, we watched the number of cases skyrocket in April and May of last year (see chart below). While a repeat performance is far from guaranteed, it is notable that the number of cases this year in the first quarter of the year is even higher than in 2014.
With nearly 1,000 cases reported out of Saudi Arabia alone, and a roughly 40% fatality rate, MERS – over the past three years – has `outperformed’ (in terms of # of people infected, deaths, and h-2-h `clusters’) all of the avian flu strains we’ve been watching (H5N1, H7N9, H5N6, H10N8, etc.) around the globe combined.
While impressive metrics, what these numbers can’t tell us is which of these viruses – if any – have the `legs’ to spark a global health crisis.
Influenza viruses have a long, if infrequent history of sparking pandemics, and novel strains are always viewed with concern. But our experience with virulent coronaviruses is far less extensive, with basically only the `close-but-no-cigar’ SARS outbreak of 2003 to go on (see SARS and Remembrance).
Comparisons between SARS and MERS are inevitable given that both are coronaviruses, both probably originated in bats but were believed spread to humans via an intermediate host, both cause severe respiratory syndromes, and both are easily spread in a hospital environment.
But they also differ in some fundamental ways.
- SARS had a fatality ratio of roughly 10% while MERS has been fatal in about 40% of hospitalized cases
- SARS had an R0 (Basic Reproductive Number) estimated between 2.0-3.0 while MERS remains < 1.0
- SARS burned intently for about 8 months and died out, while MERS has been slowly accelerating for 3 years
- Half of SARS cases were under the age of 50, while the vast majority of MERS cases are over the age of 50
- Unlike SARS which was fairly evenly divided, MERS cases are (for reasons not yet known) heavily skewed towards males
With April – and a possible repeat of last year’s surge – just around the corner, the World Health Organization has released an updated summary on the MERS virus, which includes some very useful graphics.
While many questions about its transmission in the community remain, the basic epidemiology of the virus and demographics of its victims appears unchanged.
This from WHO’s Eastern Mediterranean Regional Office (EMRO).
Update on Middle East respiratory syndrome, March 2015
Highlights
- A total of 967 laboratory-confirmed cases of MERS-CoV, including 379 deaths (case-fatality rate 39%) were reported from Saudi Arabia. Of these, a total of 145 cases, including 58 deaths (case-fatality rate 40%), were reported in 2015 to date.
- The epidemiological and demographic characteristics of the disease do not show any significant difference. The majority of cases continue to be male and the most affected age group among primary cases are those between 50 and 59 years of old.
- Nosocomial outbreaks in hospitals, though smaller in size and risk, as compared to the past, have been reported from Riyadh, Qassem, Al-Jouf and eastern Regions.
- Since the last big hospital outbreak in Jeddah in 2014, nosocomial infection reported among health care workers have continued to decline (from as high as 25% to 12%).