# 7487
Although West Nile Virus (WNV) activity was high across much of the country in 2012, the hardest hit area was Dallas County, Texas, where at least 19 people died from the severe form of this mosquito borne infection called Neuroinvasive West Nile Disease.
Mild cases – called West Nile Fever – often go undiagnosed, with probably only 2%-3% being identified. You’ll find some of my coverage of last year’s outbreak in Texas in the following blogs:
CDC Telebriefing on West Nile Virus
Updating the Texas West Nile Outbreak
Dallas West Nile Update
Nationally, the CDC reported last May:
Final 2012 West Nile virus update:
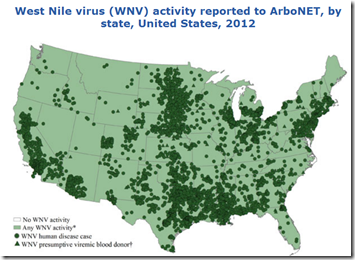
In 2012, all 48 contiguous states, the District of Columbia, and Puerto Rico reported West Nile virus infections in people, birds, or mosquitoes. A total of 5,674 cases of West Nile virus disease in people, including 286 deaths, were reported to CDC. Of these, 2,873 (51%) were classified as neuroinvasive disease (such as meningitis or encephalitis) and 2,801 (49%) were classified as non-neuroinvasive disease. The numbers of neuroinvasive, non-neuroinvasive, and total West Nile virus disease cases reported in 2012 are the highest since 2003.
It is estimated that only about 20% of the people who are infected with WNV develop symptoms, and the vast majority of those only experience a mild flu-like illness. Accordingly, mild, asymptomatic, or non-neuroinvasive infections are likely vastly undercounted.
The more severe `neuroinvasive’ form of WNV can produce symptoms that include headache, stiff neck, confusion, coma, convulsions, and even paralysis.
According to the CDC’s WEST NILE SYMPTOMS Q&A page.
What are the symptoms of West Nile virus disease?
No symptoms in most people. Most people (70-80%) who become infected with West Nile virus do not develop any symptoms.
Febrile illness in some people. About 1 in 5 people who are infected will develop a fever with other symptoms such as headache, body aches, joint pains, vomiting, diarrhea, or rash. Most people with this type of West Nile virus disease recover completely, but fatigue and weakness can last for weeks or months.
Severe symptoms in a few people. Less than 1% of people who are infected will develop a serious neurologic illness such as encephalitis or meningitis (inflammation of the brain or surrounding tissues). The symptoms of neurologic illness can include headache, high fever, neck stiffness, disorientation, coma, tremors, seizures, or paralysis.
Recovery from severe disease may take several weeks or months. Some of the neurologic effects may be permanent. About 10 percent of people who develop neurologic infection due to West Nile virus will die.
Which brings us to a research article (which you can read in its entirety) that appeared in JAMA yesterday on the Dallas epidemic, that finds correlations between an unusually mild winter, the early detection of WNV bearing mosquitoes, and the likelihood of seeing a major WNV outbreak.
The 2012 West Nile Encephalitis Epidemic in Dallas, Texas FREE
Wendy M. Chung, MD, SM1; Christen M. Buseman, PhD, MPH1; Sibeso N. Joyner, MPH1; Sonya M. Hughes, MPH1; Thomas B. Fomby, PhD4; James P. Luby, MD2; Robert W. Haley, MD3
Conclusions and Relevance Large West Nile virus epidemics in Dallas County begin early after unusually warm winters, revisit similar geographical distributions, and are strongly predicted by the mosquito vector index. Consideration of weather patterns and historical geographical hot spots and acting on the vector index may help prevent West Nile virus–associated illness.
The outbreak, which reached its peak in early August, was eventually brought under control after aerial spraying began in week 32 (see chart below).
Despite some initial public concerns over the use of aerial insecticides, surveillance of local emergency rooms did not detect any increase in ER visits for respiratory symptoms or rashes following airborne spraying.
In addition to the study you’ll find a short (4 minute) video by Dr. WM Chung, lead author of the study.
Although it is too early in the summer to know what kind of WNV season 2013 will bring, the CDC’s DVBID reports the following activity:
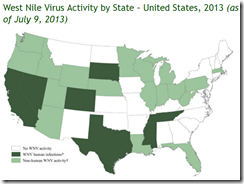
Preliminary Maps & Data for 2013
As of July 9, 2013, 25 states and the District of Columbia have reported West Nile virus infections in people, birds, or mosquitoes. A total of 14 cases of West Nile virus disease in people, including two deaths, have been reported to CDC. Of these, five (36%) were classified as neuroinvasive disease (such as meningitis or encephalitis) and nine (64%) were classified as non-neuroinvasive disease.
Which is why health departments across the nation urge people to follow the `5 D’s’ of mosquito protection: