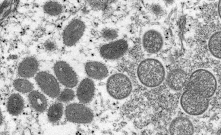
Monkeypox Virus - Credit CDC PHIL
#17,086
While the number of monkeypox cases being reported in the United States continues to decline, and most cases are described as mild and self-limited, for a relatively small number of (mostly severely immunocompromised) individuals, Monkeypox infection can be a serious and even fatal disease.
Health Alert Network (HAN) No. 475 – Severe Manifestations of Monkeypox among People who are Immunocompromised Due to HIV or Other Conditions 09/29/2022 2:15 PM
This was followed up by a CDC COCA Call for clinicians (see Situational Update for Clinicians About Severe Monkeypox Virus Infections) in early October.
Yesterday the CDC's MMWR published an early release on 57 severe Monkeypox cases reported to the CDC over a recent 60 day period, detailing three representative cases. Most of these cases involved black men with AIDS, a quarter of them homeless, many of whom experienced delays in getting treatment.
Twelve of the 57 patients died, with Monkeypox listed as a contributing cause of death in at least 5 cases (others are still under investigation).
This is a grim but illuminating report that reminds us that there is often a hidden burden of disease and suffering - particularly among those with chronic health problems, or who live on the margins of society - that rarely makes the evening news.
Severe Monkeypox in Hospitalized Patients — United States, August 10–October 10, 2022
Early Release / October 26, 2022 / 71
Maureen J. Miller, MD1,*; Shama Cash-Goldwasser, MD1,2,3,*; Grace E. Marx, MD1; Caroline A. Schrodt, MD1; Anne Kimball, MD1; Kia Padgett, MPH1; Rebecca S. Noe, MPH1; David W. McCormick, MD1,2; Joshua M. Wong, MD1,2; Sarah M. Labuda, MD1; Brian F. Borah, MD1,2,4; Isaac Zulu, MD1; Amimah Asif, MBBS1; Gurpreet Kaur, MD1,2; Janet M. McNicholl, MD1; Athena Kourtis, MD1; Andrew Tadros, MD, PhD1; Sarah Reagan-Steiner, MD1; Jana M. Ritter, DVM1; Yon Yu, PharmD1; Patricia Yu, MPH1; Rachel Clinton, MS1; Corrine Parker, PharmD1; Eleanor S. Click, MD, PhD1,2; Johanna S. Salzer, DVM1; Andrea M. McCollum, PhD1; Brett Petersen, MD1; Faisal S. Minhaj, PharmD1,2; Ericka Brown, MD5; Michael P. Fischer, MD6; Robert L. Atmar, MD7; Andrew R. DiNardo, MD7; Ya Xu, MD, PhD7; Cameron Brown, PhD7; Jerry Clay Goodman, MD7; Ashley Holloman, MD7; Julia Gallardo, MD7; Hanna Siatecka, MD7; Georgia Huffman, MD7; John Powell, MD7; Philip Alapat, MD7; Pralay Sarkar, MD7; Nicola A. Hanania, MD7; Or Bruck, MD7; Steven D. Brass, MD7; Aneesh Mehta, MD8; Alexandra W. Dretler, MD9; Amanda Feldpausch, DVM10; Jessica Pavlick, DrPH10; Hillary Spencer, MD2,11; Isaac Ghinai, MBBS11; Stephanie R. Black, MD11,12; Laura N. Hernandez-Guarin, MD12; Sarah Y. Won, MD12; Shivanjali Shankaran, MD12; Andrew T. Simms, MD12; Jemma Alarcón, MD2,13; Jesse G. O’Shea, MD1; John T. Brooks, MD1; Jennifer McQuiston, DVM1; Margaret A. Honein, PhD1; Siobhán M. O’Connor, MD1; Kevin Chatham-Stephens, MD1; Kevin O’Laughlin, MD1; Agam K. Rao, MD1; Elliot Raizes, MD1; Jeremy A. W. Gold, MD1,†; Sapna Bamrah Morris, MD1,†; CDC Severe Monkeypox Investigations Team (VIEW AUTHOR AFFILIATIONS)View suggested citation
Summary
What is already known about this topic?
Severe manifestations of monkeypox in immunocompromised persons have been observed in previous outbreaks.
What is added by this report?
During August–October 2022, CDC provided clinical consultation for 57 hospitalized patients with severe manifestations of monkeypox, most of whom were Black men with AIDS. Delays were observed in initiation of monkeypox-directed therapies. Twelve patients died, and monkeypox was a cause of death or contributing factor in five patients to date, with several other deaths still under investigation.
What are the implications for public health practice?
Clinicians should consider early treatment with available therapeutics for those at risk for severe monkeypox disease, particularly patients with AIDS. Engaging all persons with HIV in care remains a critical public health priority.
As of October 21, 2022, a total of 27,884 monkeypox cases (confirmed and probable) have been reported in the United States.§ Gay, bisexual, and other men who have sex with men have constituted a majority of cases, and persons with HIV infection and those from racial and ethnic minority groups have been disproportionately affected (1,2). During previous monkeypox outbreaks, severe manifestations of disease and poor outcomes have been reported among persons with HIV infection, particularly those with AIDS (3–5).This report summarizes findings from CDC clinical consultations provided for 57 patients aged ≥18 years who were hospitalized with severe manifestations of monkeypox¶ during August 10–October 10, 2022, and highlights three clinically representative cases. Overall, 47 (82%) patients had HIV infection, four (9%) of whom were receiving antiretroviral therapy (ART) before monkeypox diagnosis. Most patients were male (95%) and 68% were non-Hispanic Black (Black). Overall, 17 (30%) patients received intensive care unit (ICU)–level care, and 12 (21%) have died.As of this report, monkeypox was a cause of death or contributing factor in five of these deaths; six deaths remain under investigation to determine whether monkeypox was a causal or contributing factor; and in one death, monkeypox was not a cause or contributing factor.** Health care providers and public health professionals should be aware that severe morbidity and mortality associated with monkeypox have been observed during the current outbreak in the United States (6,7), particularly among highly immunocompromised persons.Providers should test all sexually active patients with suspected monkeypox for HIV at the time of monkeypox testing unless a patient is already known to have HIV infection. Providers should consider early commencement and extended duration of monkeypox-directed therapy†† in highly immunocompromised patients with suspected or laboratory-diagnosed monkeypox.§§ Engaging all persons with HIV in sustained care remains a critical public health priority.
(SNIP)
Discussion
Although most monkeypox cases during the ongoing outbreak have been self-limited (2,8), this report highlights the occurrence of severe manifestations of monkeypox in the United States, particularly in persons with AIDS. In this cohort of patients hospitalized with monkeypox and for whom clinicians or jurisdictions sought consultations with CDC, nearly one third (30%) received ICU-level care, and 21% of patients died, including several deaths that remain under investigation to determine the cause of death. Most patients eventually received tecovirimat, but some experienced delays of up to 4 weeks between initial care-seeking for monkeypox symptoms and initiation of monkeypox-directed therapy. For patients with suspected or laboratory-diagnosed monkeypox who are at risk for severe disease (particularly those with AIDS and other types of severe immunocompromise), health care providers should consider starting monkeypox-directed therapy early, potentially before receipt of monkeypox testing results or before severe manifestations are observed. In patients with severe disease, or with ongoing disease despite treatment, providers should consider extending tecovirimat treatment beyond 14 days and escalating therapy to include cidofovir or VIGIV if clinically indicated (9). For patients with HIV disease who are not on ART, clinicians should initiate ART as soon as possible, regardless of CD4 cell count.**** Health care providers should test all sexually active patients with suspected monkeypox for HIV at the time of testing for monkeypox unless a patient is already known to have HIV infection.
Most patients in this cohort were Black men, and nearly one quarter of cases occurred in persons experiencing homelessness. These findings likely reflect inequities in access to resources for the prevention, early diagnosis, and treatment of HIV infection, as well as missed opportunities to engage groups that have been socially or economically marginalized.†††† Public health outreach should strive to engage all persons with HIV infection in care and to increase access to monkeypox vaccination, diagnosis, and treatment. To accomplish these goals, it is critical to leverage existing HIV and sexually transmitted infection program resources and prioritize communities disproportionately affected by HIV (1). Collaboration with homeless services providers can help engage persons who are experiencing homelessness in prevention and treatment services for HIV and monkeypox.
The findings in this report are subject to at least four limitations. First, cases were passively identified by CDC through consultations requested by clinicians or jurisdictions and might not be representative of all patients with severe monkeypox. Second, this report only included outcomes occurring during the study period; therefore, deaths occurring after this period were not included. Third, observed morbidity and mortality might have been related to factors apart from or in addition to monkeypox, including HIV-related opportunistic infections. Finally, conclusions about the effectiveness of monkeypox treatments cannot be inferred from these observational data.
The occurrence of severe manifestations of monkeypox in patients who were most commonly immunocompromised because of AIDS highlights the importance of engaging all persons with HIV in sustained care and ending the HIV epidemic. Clinicians should consider close clinical monitoring, early treatment with available medical countermeasures, and extension or escalation of therapy as indicated in patients with or at risk for severe monkeypox. Ensuring equitable access to resources for the diagnosis, treatment, and prevention of HIV and monkeypox remains a vital public health priority.