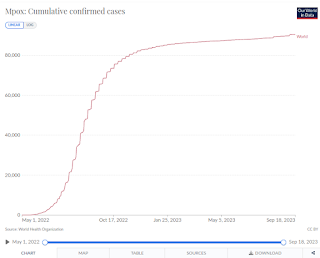
Cumulative Mpox Cases - Credit Our World In Data
#17,682
After simmering for decades in west and central Africa, 16 months ago Monkeypox (aka `Mpox') burst onto the international scene (see WHO Europe: Statement By WHO Regional Director On Monkeypox Outbreak Investigation) following reports of cases in 12 non-endemic countries.
In July of 2022 the WHO Director Declared Monkeypox A Public Health Emergency Of International Concern (PHEIC). New case reports peaked in the fall of 2022, and continue today at a much reduced level.
Although the WHO discontinued their PHEIC status for Mpox last May, concerns over the future spread, and evolution, of this virus remain. Many countries do not screen for, or publicly report cases, and the true incidence of the disease is hard to quantify.
While many were surprised by this sudden epidemic, Monkeypox's spread out of Africa had been long predicted (see EID Journal: Reemergence of Human Monkeypox and Declining Population Immunity - Nigeria, 2017–2020).
Like all viruses, Mpox continues to evolve and diversify, as discussed in the 2014 EID Journal article Genomic Variability of Monkeypox Virus among Humans, Democratic Republic of the Congo, where the authors cautioned:
Small genetic changes could favor adaptation to a human host, and this potential is greatest for pathogens with moderate transmission rates (such as MPXV) (40). The ability to spread rapidly and efficiently from human to human could enhance spread by travelers to new regions.
On a 2020 report, published by the Bulletin of the World Health Organization, researchers warned that our waning immunity to smallpox put society at greater risks of seeing Monkeypox epidemics (see WHO: Modelling Human-to-Human Transmission of Monkeypox).
While the vast majority of Monkeypox cases have occurred among men who reported recent male-to-male sexual contact (MMSC), a small - but notable - number of cases reported no such activity.
A recent MMWR report (Possible Exposures Among Mpox Patients Without Reported Male-to-Male Sexual Contact). suggested other possible routes - including fomites - might be a factor.
Over the summer of 2022 we saw several studies which detailed extensive environmental contamination with the Mpox virus - both in household and hospital settings - including:
MMWR: High-Contact Object & Surface Contamination in a Household of Persons with Monkeypox Virus Infection
EID Journal: Environmental Persistence of Monkeypox Virus on Surfaces in A Household
Eurosurveillance: Surface Contamination in Hospital Rooms Occupied by Patients Infected with Monkeypox
This has implications both for health care workers, and for those who share a residence with someone who is infected, along with wildlife which could be conceivably exposed via wastewater (see WOAH: How Monkeypox Could Spill Back To Animals From Humans).
Research
Stability of Monkeypox Virus in Body Fluids and Wastewater
Claude Kwe Yinda1, Dylan H. Morris1, Robert J. Fischer, Shane Gallogly, Zachary A. Weishampel, Julia R. Port, Trenton Bushmaker, Jonathan E. Schulz, Kyle Bibby, Neeltje van Doremalen, James O. Lloyd-Smith, and Vincent J. Munster
Abstract
An outbreak of human mpox infection in nonendemic countries appears to have been driven largely by transmission through body fluids or skin-to-skin contact during sexual activity. We evaluated the stability of monkeypox virus (MPXV) in different environments and specific body fluids and tested the effectiveness of decontamination methodologies.
MPXV decayed faster at higher temperatures, and rates varied considerably depending on the medium in which virus was suspended, both in solution and on surfaces. More proteinaceous fluids supported greater persistence. Chlorination was an effective decontamination technique, but only at higher concentrations. Wastewater was more difficult to decontaminate than plain deionized water; testing for infectious MPXV could be a helpful addition to PCR-based wastewater surveillance when high levels of viral DNA are detected.
Our findings suggest that, because virus stability is sufficient to support environmental MPXV transmission in healthcare settings, exposure and dose-response will be limiting factors for those transmission routes.
(SNIP)
Discussion
Different studies investigating the stability of viruses of the genus Orthopoxvirus (family Poxiviridae) have arrived at similar conclusions as this study. Prolonged variola stability has been reported in scabs, vesicle and pustule fluids, lymph system, and purulent sores of patients (18). Also, investigations of variola in raw cotton and vaccinia in storm water and feces showed that a few virus particles may survive for long periods of time (18–21).
Only a few studies have tested the stability of MPXV. An experimental study conducted on MPXV aerosol indicated the virus could remain viable in aerosol form for a prolonged period (22). Two other studies measuring stability and inactivation of MPXV showed the virus could be efficiently inactivated by alcohol- and aldehyde-based surface disinfectants. When World Health Organization‒recommended alcohol-based hand rub solutions were used to test disinfection, MPXV displayed greater stability than all other emerging or reemerging enveloped viruses (23,24).
We found that MPXV indeed shows strong environmental persistence on surfaces and in solution. MPXV in some media (DMEM with human saliva, urine, and feces) showed clear biphasic decay on surfaces but not in others (blood, semen, and serum). The observed biphasic decay was indicative of stability kinetics differing from the virus initially deposited on surfaces in a liquid solution to virus remaining after macroscopic evaporation of the solution. Stability also varied depending on the various MPXV-containing fluids and wastewater we tested. MPXV persisting in clinical specimens (25–27) or tissues also suggested fluid-dependent rates of decay. More proteinaceous solutions, such as blood, serum, and semen, favored virus stability. We confirmed experimentally that the protective effect of serum was directly proportional to the concentration of serum. That finding was consistent with observations from other recent studies that environmental inactivation of viruses can be slowed by proteins in the solution and is strongly dependent on physicochemical properties of the medium (16).
Environmental risk assessment has typically focused on properties of the ambient environment (temperature, humidity, surface type for fomite transmission, ventilation rate for airborne transmission). Taken together with previous work on other viruses, our results suggest that route and type of contamination should also be considered, because viability of viruses may also depend on the body fluids from which they are shed. That factor may partly account for variability in persistence of environmental MPXV contamination on different surfaces (11) and in discrepancies between the longevity of MPXV on cotton in this study compared with results from epidemiologic investigations in which exudate (vesicular or pustular fluids) provided more virus-protective environments (18).
So far, of the many cases reported among healthcare workers, only a few have been occupationally acquired (28–32), suggesting that risk for workplace transmission of MPXV to healthcare workers is notably low. In addition, many environmental surfaces are regularly exposed to UV light and common household disinfectants, which decrease viral infectivity. Nevertheless, persistence of MPXV in the environment suggests that precautions are required to avoid environmental and nosocomial transmission, in particular in hospital settings.
MPXV transmission and spread through sexual contact, especially among MSM, has been confirmed. That means long half-lives of viable MPXV in blood and semen increase risk of transmission through fluid exchange or skin-to-skin contact during sexual activity. Potential long-term viability in semen presents further implications for viral load in infected persons and for duration of infectiousness even after viral replication stops. Genetic material from other viruses, including Zika and Ebola, has been detected in semen months or years after initial infection, but how this relates to MPXV infectivity remains an open question (33). Estimated viral half-lives in our work are consistent with infectious MPXV remaining in semen for weeks after virus replication ends, as reported elsewhere (34,35). It should be noted however, that in patient blood, so far only DNA has been detected, and what roles blood and serum can play in MPXV transmission remains unclear (36).
Our finding that MPXV can remain infectious for weeks in untreated wastewater raises the potential for risk of exposure among sanitation workers, peridomestic animals, and wildlife (13). Given the suspected role of rodents as reservoirs of MPXV, this possibility raises hypothetical concerns about zoonotic reservoirs becoming established in previously nonendemic countries.
However, we emphasize that dilution and chemical disinfection can mitigate these risks. Because previous studies only tested for viral DNA (12,37–40), we suggest that testing for infectious MPXV could be a valuable complement to PCR-based wastewater surveillance when significant quantities of viral DNA are detected.
In conclusion, our results suggest that MPXV stability is dependent on the surface, the environmental conditions, and the matrix of the virus. Overall, we found MPXV showed long half-lives in a variety of body fluids, both in bulk solutions and when deposited wet then allowed to dry on common clinical and residential surfaces, and half-lives approaching a week in untreated wastewater. Our findings suggest that, because virus stability is sufficient to support environmental or fomite transmission of MPXV, exposure and dose-response will be limiting factors for those transmission routes.
Dr. Yinda is a postdoctoral research fellow in the Laboratory of Virology of the National Institute of Allergy and Infectious Diseases. He is interested in emerging viruses and their transmission potential. Dr. Morris is a postdoctoral researcher in the Department of Ecology and Evolutionary Biology at the University of California, Los Angeles. He is interested in quantitative models of virus ecology and evolution.
While Mpox has largely disappeared from the news cycle - replaced by more `clickable' headlines - the virus quietly continues its world tour. As it spreads from host-to-host, additional evolutionary changes seem likely (see Evolution of monkeypox virus from 2017 to 2022: In the light of point mutations).
Since the eradication of smallpox in the 1970s, there is a general feeling that poxviruses are a thing of the past, a relic of the 20th century.
Admittedly, Mpox may not have the `right stuff' today to spark a major crisis, but viruses are constantly evolving and adapting, often in unpredictable ways.
And nature is nothing if not persistent.