Credit CDC
# 8858
With MERS cases dwindling, and H7N9 and H5N1 basically in hibernation until fall, our attentions this summer have been focused largely on vector borne diseases that tend to flourish during warm weather months. And three we are watching closely – WNV, Dengue & Chikungunya – are all relatively recent arrivals to the United States.
- West Nile Virus arrived in North American in 1997 and has since become endemic across the United States and into Canada (see WNV: The Economic Costs Of An Invasive Arbovirus).
- Dengue fever has made exploratory incursions into Florida (see MMWR: Dengue Fever In Key West) & Texas over the past few years, and and only last fall resulted in a case of Locally Acquired Dengue In New York City.
- Locally transmitted Chikungunya was only first reported last week (in Florida).
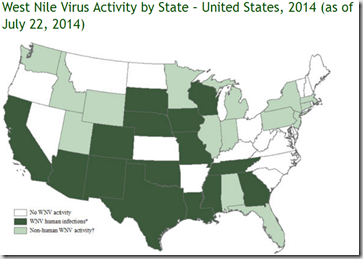
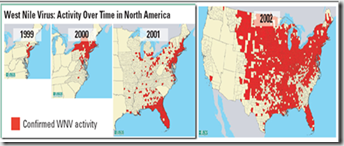
Over just a few years, WNV was able to spread from New York City, to every state in the lower 48. In 2012, it caused nearly 3,000 cases of neuroinvasive WNV, and 286 deaths (see DVBID: 2012 Record Number Of West Nile Fatalities) – while the number of milder West Nile Fever cases probably exceeded 100,000.
From the USGS Factsheet on West Nile Virus
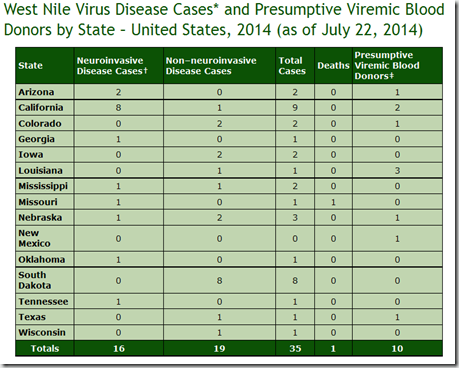
Each summer the CDC produces weekly surveillance reports on WNV activity (in humans, birds, and animals). And while these reports tend to lag behind actual events by a week or so (fatalities even more so, since some cases may be hospitalized for weeks before succumbing), they give us an excellent idea of how the WN season is progressing around the country.
While each WNV season varies as to its intensity and outbreak timing, so far we’ve not seen huge numbers of cases reported. It is, however, usually the months of August and September that tells the tale.
Neuroinvasive cases (which present with meningitis, encephalitis, or flaccid Paralysis), while less common, are severe enough that they nearly always result in hospitalization and diagnosis, and so they are considered the best indicator of the scope of each year’s epidemic. The number of `non-neuroinvasive’ cases counted is considered to represent only 1%-3% of the total.
Unlike Unlike Chikungunya and Dengue, which primarily affect humans and non-human primates – WNV is mainly a disease of birds – which gives the virus a large natural reservoir to over winter in. Humans and horses are considered `incidental’ infections (see WNV vs CHIKV: A Host Of Differences).
Dengue – which has increased tremendously around the world over the past 5 decades – has literally exploded in the Western Hemisphere since the year 2000 (see PAHO Five-fold increase in dengue cases in the Americas over the past decade), but thus far, has only made small inroads into North America.
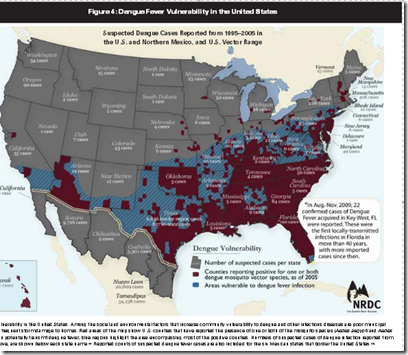
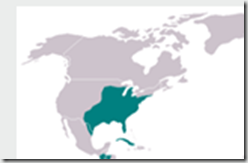
In 2009 the Natural Resources Defense Council (NRDC) released a report outlining the risks that Dengue could re-establish itself in North America, that included this map showing the areas of the United States that are vulnerable to the introduction of Dengue.
Northern climes are far less likely to see dengue take hold than say, Florida or Southern Texas. Still, in the 18th and 19th century, both Malaria and Yellow Fever were endemic up and down the mid-Atlantic coast.
While we see hundreds of imported cases of dengue in the United States each year – each with at least the potential to seed local mosquito populations with the virus – so far locally acquired cases have remained rare. The lack of an abundant non-human animal reservoir for the virus is likely partly responsible.
In 2003, a CDC EID study also found that economics and lifestyle may have a lot to do to with our lack of locally transmitted Dengue (see Texas Lifestyle Limits Transmission of Dengue Virus).
But given the availability of two competent mosquito vectors (Aedes Aegypti & Aedes Albopictus), and repeated introductions of the virus from travelers coming from regions where the virus is endemic, our luck in this matter may not last forever.
With well over 80 million visitors each year, many coming from regions where dengue, malaria, and chikungunya are endemic, Florida is the ideal place to monitor mosquito-borne diseases coming into the United States. The most recent Florida Arbovirus Surveillance Report (week 29) illustrates these repeated introductions:
International Travel-Associated Dengue Fever Cases: One case of dengue fever was reported this week in a person that had international travel: Brevard County. In 2014, 27 travel-associated cases have been reported.
Dengue Fever Cases Acquired in Florida:No cases of locally acquired dengue fever were reported this week. In 2014, a total of one case of locally acquired dengue fever has been reported.
International Travel-Associated Chikungunya Fever Cases: Six cases of chikungunya fever were reported this week in persons that had international travel. In 2014, 87 travel-associated cases have been reported.
Chikungunya Fever Cases Acquired in Florida:Two case of locally acquired chikungunya fever were reported this week in residents of Miami-Dade and Palm Beach Counties. In 2014, a total of two cases of locally acquired chikungunya fever have been reported.
Additionally, 28 cases of International Travel-Associated Malaria have been reported in Florida in 2014. Over the past decade there have only been about a dozen locally acquired cases of Malaria in Florida.The only clusters were reported in 1996 (2 cases) and again in 2003 (8 cases) of locally acquired P. vivax malaria detected in Palm Beach County (see Multifocal Autochthonous Transmission of Malaria --- Florida, 2003).
The new kid on the block is Chikungunya, and as with Dengue before it, it is now exploding across the Caribbean. The latest PAHO numbers show 436,586 cases since the outbreak began in December, but that is likely an undercount. Hardest hit has been the Dominican Republic, accounting for more than half of the total cases reported.
As with Dengue, the virus is maintained in the human population, and spread by mosquitoes – giving hope that the same environmental and economic factors that limit the spread of Dengue in the United States may also help suppress the spread of Chikungunya.
But the unknown factor is the Aedes Albopictus mosquito – aka the `Asian Tiger’ mosquito – which ironically also only recently arrived in North America. First seen in Texas in the early 1980s (believed to have been imported on cargo ships from S.E. Asia), this aggressive biter can now be found from Florida to Maine, and swarms well into the Midwest.
In 2005 a mutation in the envelope protein gene (E1-A226V) of the Chikungunya virus was credited with allowing Aedes Albopictus or `Asian tiger’ mosquito to transmit the virus more efficiently (see A Single Mutation in Chikungunya Virus Affects Vector Specificity and Epidemic Potential), and has led to its rapid expansion across the globe.
It remains to be seen whether Chikungunya will act more like West Nile Virus – and become entrenched across large swaths of the United States – or act more like Dengue, and require constant reseeding from international travelers, only causing small localized clusters of infection.
The good news is that these mosquito-borne illnesses (and others, including SLEV, EEE, etc.) are largely preventable.
Florida’s Health department reminds people to always follow the `5 D’s’: