# 9801
In the wake of this weekend’s announced imported MERS case in Germany (see Germany Reports Imported MERS Case - ex UAE), and barely two weeks since their last update, the ECDC has published their 15th Rapid Risk Assessment on the novel coronavirus threat to the EU.
Main conclusions and recommendations
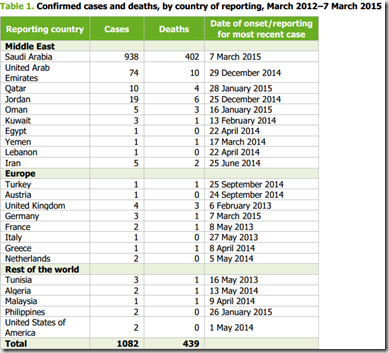
- Since April 2012 and as of 7 March 2015, 1 082 cases (including 439 deaths) of Middle East respiratory syndrome coronavirus (MERS-CoV) have been reported by local health authorities worldwide.
- The incidence of cases has been rising in the Arabian Peninsula in the past month. A similar pattern has been observed in previous years.
- The majority of MERS-CoV cases are still being reported from the Arabian Peninsula, specifically from Saudi Arabia, and all cases have epidemiological links to the outbreak epicentre. The source of MERSCoV infection and the mode of transmission have still not been confirmed.
- The latest importation of a case to Germany from the United Arab Emirates demonstrates the continued risk of case importation to Europe after exposure in the Middle East, especially in the context of the seasonal upsurge of cases currently observed in Saudi Arabia. However, the risk of sustained human-tohuman transmission in Europe remains very low.
- Taking into account the latest development with respect to MERS-CoV, ECDC's conclusion continues to be that the MERS-CoV outbreak poses a low risk to the EU, as stated in the previous update of ECDC's Rapid Risk Assessment on MERS-CoV, dated 23 February 2015 [1].
- National healthcare providers and public health institutions should remain prepared for a possible imported case in the EU/EEA.
- WHO recommends that probable and confirmed cases should be admitted to adequately ventilated single rooms or airborne precaution rooms. Healthcare workers caring for probable or confirmed cases of MERS-CoV infection should use contact and droplet precautions (medical mask, eye protection – i.e. goggles or face shield – gown and gloves [2]) in addition to standard precautions. Airborne precautions should be applied when performing aerosol-generating procedures.
- The advice for travellers to affected areas remains the same as in previous ECDC risk assessments.
As we’ve come to expect from the ECDC, we are also provided with a number of excellent charts, graphs, and maps along with a detailed epidemiological discussion of the virus.
Since April 2012 and as of 7 March 2015, 1 082 cases (including 439 deaths) of MERS-CoV have been reported by
health authorities worldwide (Figure 1).Current situation in Saudi Arabia
Since the last rapid risk assessment on 24 February 2015, Saudi Arabia has reported 39 additional cases and 20 deaths. The cases were reported from Riyadh (25), Khobar (3), Buaydah (3), Jeddah (2), Al Jawf (1) Hofuf (1), Najran (1), Qweyah (1), Shakra (1) and Unazah (1). Of the 36 cases with known age and gender, 67% (n=24) were male. The mean age was 56 years, ranging from 24 to 83 years for the 36 cases. Nine of the 39 cases were classified as nosocomial transmission, while five are currently under investigation for possible nosocomial transmission. Seven of the 39 cases were healthcare workers. Three of the 39 cases reported contact with animals, one of these cases reported camel contact.
As we’ve discussed often in the past (see here, here, and here), the lack of a well mounted case-control study by Saudi Arabia puts them, and the rest of the world, in the unenviable position of not fully understanding how this virus is spreading among humans.
We know a small number of cases appear to be linked to animal (mostly camel) exposure, and a sizable chunk have been exposed at healthcare facilities, but for the vast majority of cases the route of exposure is unknown.
While the epicenter, and vast majority of this spring’s MERS activity will likely remain in the Middle East, we should expect that additional cases will be exported from the region, and that they can literally turn up practically anywhere in the world.