#17,423
Although COVID infection has been tentatively linked to a variety of short and long-term sequelae (see EID Journal: Postacute Sequelae of SARS-CoV-2 in University Setting), we are just beginning to understand the scope of its impact on human health.
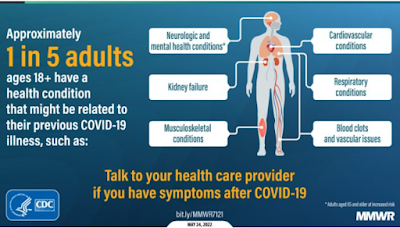
Post-COVID sequelae may include cardiovascular, renal, pulmonary, neurological, and endocrine disorders. A few (of many) studies include:
Nature: Long-term Cardiovascular Outcomes of COVID-19
BMJ: Elevated Risk Of Blood Clots Up To 6 Months After COVID Infection
Nature: Long-term Neurologic Outcomes of COVID-19
Neurology: Incidence of Epilepsy and Seizures Over the First 6 Months After a COVID-19 Diagnosis: A Retrospective Cohort Study
Making matters worse, evidence suggests that repeated infections increase the odds of developing post-COVID complications (see Nature: Acute and Postacute Sequelae Associated with SARS-CoV-2 Reinfection).
While the acute phase of Omicron infection is generally mild, three months ago the AMA released a statement (see What doctors wish patients knew about COVID-19 reinfection) calling reinfection `problematic' and equating it to `. . . playing Russian roulette" with the virus.
Increasingly, we've seen reports suggesting there is an increased risk of developing Diabetes (Type 1 or 2) following a COVID infection. These reports go back well over a year, and include:
- Overall, those who tested positive for COVID were 17% more likely to develop diabetes in the ensuing 8 months, but that number rose to 22% for males
- Those admitted to a hospital for COVID were 2.4 times more likely to develop diabetes
- Those who were admitted to intensive care were 3.29 times more likely to develop diabetes
I've only posted some excerpts, so follow the link to read it in its entirety. I'll have a brief postscript after the break.
Original Investigation
Infectious Diseases
April 18, 2023
Association of COVID-19 Infection With Incident Diabetes
Key Points
Question
Is SARS-Cov-2 infection associated with incident diabetes?
Findings
In this cohort study of 629 935 individuals tested for SARS-CoV-2, the hazard of incident diabetes was significantly higher among individuals who tested positive for SARS-CoV-2 infection than those who tested negative. The fraction of incident diabetes cases attributable to SARS-CoV-2 infection was 3% to 5%.
Meaning
This study found that SARS-CoV-2 infection was associated with a higher risk of diabetes, suggesting that these infections may have contributed to an excess burden of diabetes at the population level.
Abstract
Importance SARS-CoV-2 infection may lead to acute and chronic sequelae. Emerging evidence suggests a higher risk of diabetes after infection, but population-based evidence is still sparse.
Objective To evaluate the association between COVID-19 infection, including severity of infection, and risk of diabetes.
Design, Setting, and Participants This population-based cohort study was conducted in British Columbia, Canada, from January 1, 2020, to December 31, 2021, using the British Columbia COVID-19 Cohort, a surveillance platform that integrates COVID-19 data with population-based registries and administrative data sets. Individuals tested for SARS-CoV-2 by real-time reverse transcription-polymerase chain reaction (RT-PCR) were included. Those who tested positive for SARS-CoV-2 (ie, those who were exposed) were matched on sex, age, and collection date of RT-PCR test at a 1:4 ratio to those who tested negative (ie, those who were unexposed). Analysis was conducted January 14, 2022, to January 19, 2023.
Exposure SARS-CoV-2 infection.
Main Outcomes and Measures The primary outcome was incident diabetes (insulin dependent or not insulin dependent) identified more than 30 days after the specimen collection date for the SARS-CoV-2 test with a validated algorithm based on medical visits, hospitalization records, chronic disease registry, and prescription drugs for diabetes management. Multivariable Cox proportional hazard modeling was performed to evaluate the association between SARS-CoV-2 infection and diabetes risk. Stratified analyses were performed to assess the interaction of SARS-CoV-2 infection with diabetes risk by sex, age, and vaccination status.
Results Among 629 935 individuals (median [IQR] age, 32 [25.0-42.0] years; 322 565 females [51.2%]) tested for SARS-CoV-2 in the analytic sample, 125 987 individuals were exposed and 503 948 individuals were unexposed. During the median (IQR) follow-up of 257 (102-356) days, events of incident diabetes were observed among 608 individuals who were exposed (0.5%) and 1864 individuals who were not exposed (0.4%).
The incident diabetes rate per 100 000 person-years was significantly higher in the exposed vs nonexposed group (672.2 incidents; 95% CI, 618.7-725.6 incidents vs 508.7 incidents; 95% CI, 485.6-531.8 incidents; P < .001). The risk of incident diabetes was also higher in the exposed group (hazard ratio [HR], 1.17; 95% CI, 1.06-1.28) and among males (adjusted HR, 1.22; 95% CI, 1.06-1.40).
The risk of diabetes was higher among people with severe disease vs those without COVID-19, including individuals admitted to the intensive care unit (HR, 3.29; 95% CI, 1.98-5.48) or hospital (HR, 2.42; 95% CI, 1.87-3.15). The fraction of incident diabetes cases attributable to SARS-CoV-2 infection was 3.41% (95% CI, 1.20%-5.61%) overall and 4.75% (95% CI, 1.30%-8.20%) among males.
Conclusions and Relevance In this cohort study, SARS-CoV-2 infection was associated with a higher risk of diabetes and may have contributed to a 3% to 5% excess burden of diabetes at a population level.
You'll find an accompanying editorial at:
COVID-19 and Incident Diabetes—Recovery Is Not So Sweet After All
Pamela B. Davis, MD, PhD1; Rong Xu, PhD2
After three long years of a pandemic it is understandable that governments and society should want to declare victory, relegate COVID to being a `flu-like' illness, and move on with life. As a result, many people have abandoned the wearing of masks and staying updated with the latest COVID booster.
But the evidence continues to suggest that normalizing COVID infection (and reinfections) will come at a cost - both to individuals - and to society as a whole.