Although it's gist had been telegraphed in the media for several weeks, yesterday the CDC unveiled their revised (and unified for Flu, RSV, COVID, etc.) respiratory virus guidelines for the public, which removes the arbitrary 5-day isolation rule for COVID.
While evidence suggests that COVID infection can be more dangerous than influenza or RSV (see blogs here, here, here, and here), it is pretty apparent that very few were adhering to the old guidelines.
COVID infections remain quite common, but between vaccines and past exposures, we tend to have less severe disease than we did 2 or 3 years ago. As a result hospitals are no longer overrun, deaths have sharply declined, and fewer people are bothering with home test kits.
COVID deaths or hospitalizations are now only rarely reported (see No News Is . . . Now Commonplace), even to the WHO.
In other words, while the threat hasn't disappeared entirely, the world has moved on. At least until the next high-impact virus emerges (see BMJ Global: Historical Trends Demonstrate a Pattern of Increasingly Frequent & Severe Zoonotic Spillover Events).
It is important to note that the CDC's new guidance still calls for staying home (and other appropriate measures) both when and after experiencing any symptomatic respiratory virus.
Below you'll find links to the new CDC guidance, followed by an excerpt from their home isolation recommendations. I'll have postscript after the break.
Respiratory Virus Guidance
This guidance is not applicable to healthcare settings. Nothing in this guidance supersedes accommodations required under federal civil rights laws.
Each year, respiratory viruses are responsible for millions of illnesses and thousands of hospitalizations and deaths in the United States. In addition to the virus that causes COVID-19, there are many other types of respiratory viruses, including flu and respiratory syncytial virus (RSV). The good news is there are actions you can take to help protect yourself and others from health risks caused by respiratory viruses.
CDC’s Respiratory Virus Guidance
This guidance provides practical recommendations and information to help people lower risk from a range of common respiratory viral illnesses, including COVID-19, flu, and RSV.
Preventing Respiratory VirusesImmunizations for Respiratory Viruses
Hygiene and Respiratory Virus Prevention
Taking Steps for Cleaner Air for Respiratory Virus Prevention
Preventing Spread of Respiratory Viruses When You’re Sick
Masks and Respiratory Virus Prevention
Physical Distancing and Respiratory Viruses
Testing and Respiratory Viruses
Special Considerations
In addition to CDC’s Respiratory Virus Guidance, there are several special considerations for people with certain risk factors for severe illness.
Risk Factors for Severe Illness from Respiratory Viruses
Older Adults
Young Children
People with Weakened Immune Systems
People with Disabilities
Pregnant People
Treatment as Prevention
Treatment is a core prevention strategy to lower risk from respiratory viruses.
Treatment of Respiratory Viruses
About the Guidance
(EXCERPT)
What is the updated guidance?
Protect Yourself from Getting Sick:
The most important thing you can do to protect yourself from COVID-19, flu, and RSV is to stay up to date on your recommended vaccines. Even when vaccines don’t prevent infection, they often tame these viruses, reducing severity, and preventing their worst outcomes, like hospitalization and death. Along with staying up-to-date on your vaccines, practicing good hygiene by covering your coughs and sneezes, washing or sanitizing your hands often, and cleaning frequently touched surfaces can help. Also, taking steps for cleaner air can help reduce the spread of respiratory viruses. This can mean bringing in fresh outside air by opening a window, purifying indoor air, or having outdoor social activities.
If You Get Sick:
Even if you practice these core prevention strategies, you may still catch a virus and develop respiratory symptoms. If that happens, the updated Guidance recommends two actions:
Step 1: Stay at home. As much as possible, you should stay home and away from others until at least 24 hours after both:
- Your symptoms are getting better overall, and
- You have not had a fever (and are not using fever-reducing medication).
This advice is similar to what has been recommended for flu for decades and will help reduce the spread of COVID-19 and other respiratory viruses during the most contagious period after infection. Not all respiratory virus infections result in a fever, so paying attention to other symptoms (cough, muscle aches, etc.) is important as you determine when you are well enough to leave home. If your symptoms are getting better, and stay better for 24 hours, you are less likely to pass your infection to others and you can start getting back to your daily routine and move on to step 2.
Step 2: Resume normal activities, and use added prevention strategies over the next five days, such as taking more steps for cleaner air, enhancing your hygiene practices, wearing a well-fitting mask, keeping a distance from others, and/or getting tested for respiratory viruses. People can choose to use these prevention strategies at any time. Since some people remain contagious beyond the “stay-at-home” period, taking added precautions can lower the chance of spreading respiratory viruses to others
People who are at higher risk for severe illness who start to feel sick should seek health care right away so that they can access testing and/or treatment. Early treatment for COVID-19 or flu may prevent severe disease in people at higher risk, even if they are up to date with their vaccines.
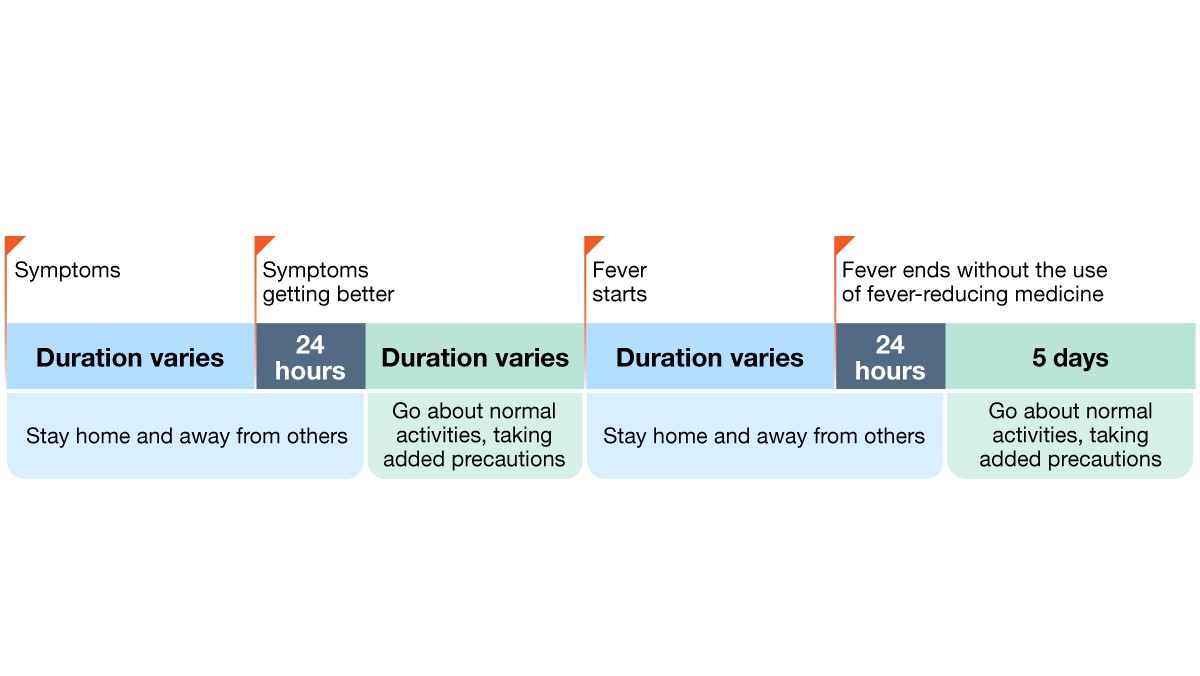
Examples
Depending on your circumstances, here are a few examples of what updated guidance could look like if you come down with a respiratory infection:
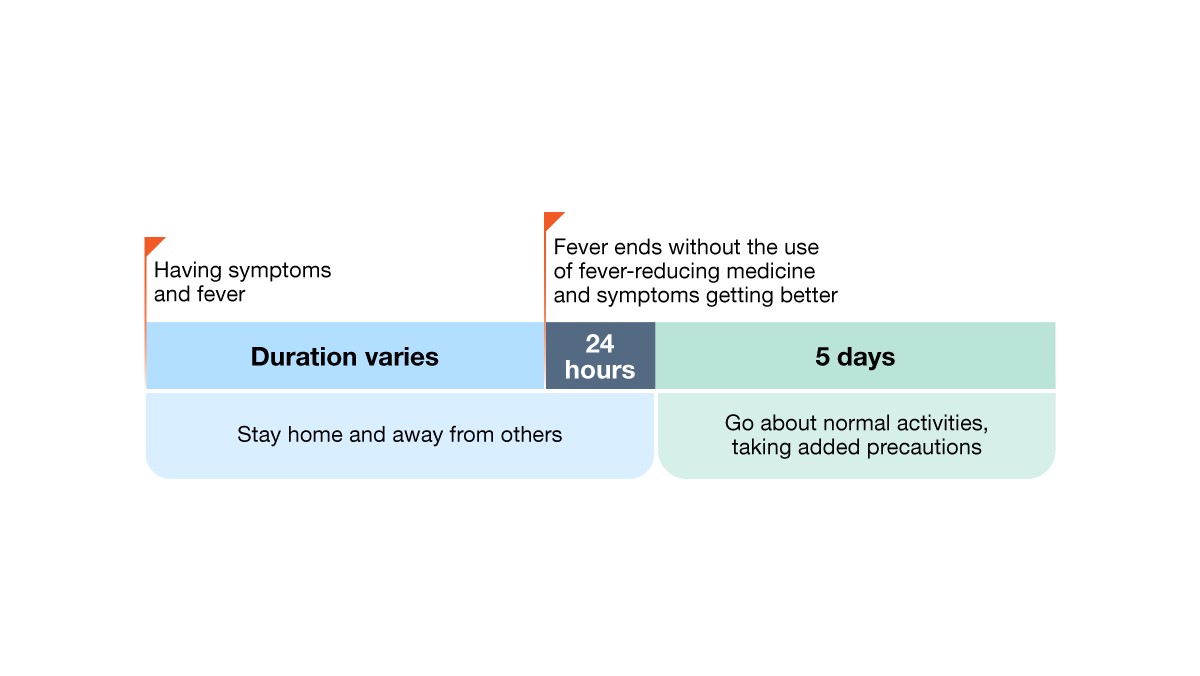
Example 1: Person with fever and symptoms.
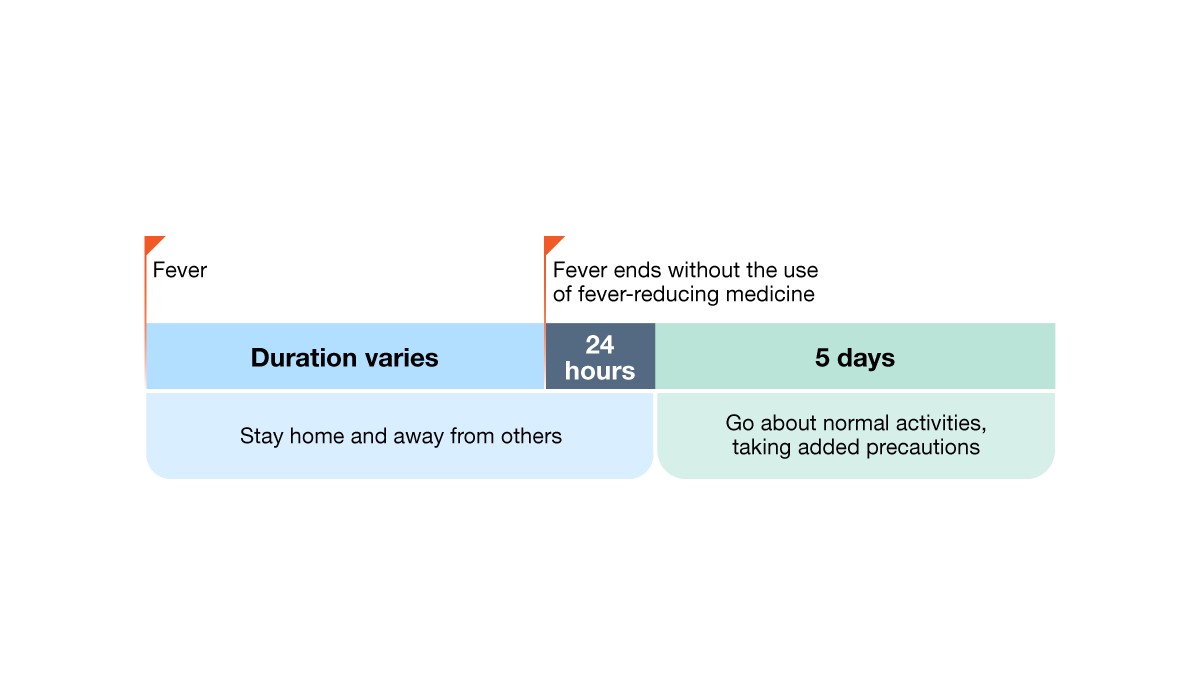
Example 2: Person with fever but no other symptoms.
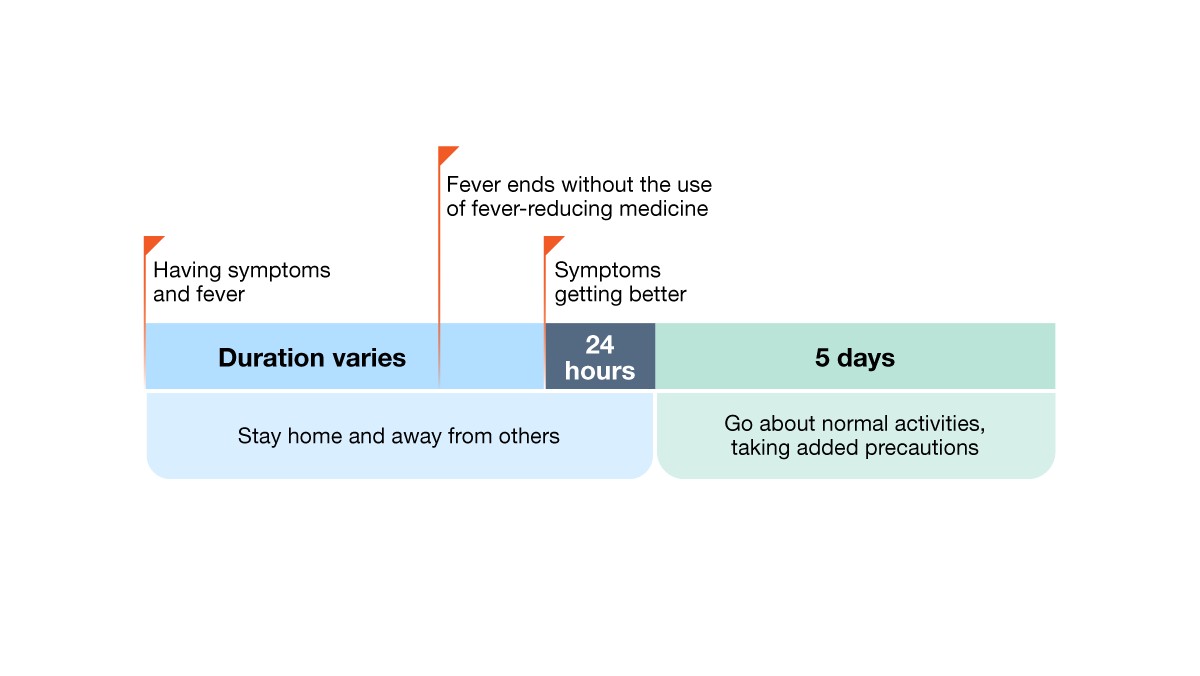
Example 3: Person with fever and other symptoms, fever ends but other symptoms take longer to improve
Compliance, even with these newly revised recommendations, is likely to be low or inconsistent. But even if everyone followed them diligently, respiratory viruses would still circulate.