Credit CDC
# 7577
Cytokines are a category of signaling molecules that are used extensively in cellular communication. They are often released by immune cells that have encountered a pathogen, and are designed to alert and activate other immune cells to join in the fight against the invading pathogen.
This cascade of immune cells rushing to the infection, if it races out of control, can overwhelm the patient. Their lungs can fill with fluid (which makes a terrific medium for a bacterial co-infection), and cells in the lungs (Type 1 & Type II Pneumocytes) can sustain severe damage.
Previously, in Swine Flu Sequelae and Cytokine Storm Warnings, we looked at some of the severe lung damage detected during the 2009 pandemic that was thought to be due to this overreaction of the immune system.
Last night Robert Roos, Editor of CIDRAP NEWS, wrote about a study that appeared this week in the American Journal of Pathology that looked at the lungs from 50 fatal cases of H1N1 during the 2009 pandemic, and their finding of "remarkably" high levels of cytokines in the lung tissue.
Robert does a terrific job explaining this research, so I’ll invite you to read his article at the link below. When you return, I’ll have some more background on the cytokine response.
Study shows cytokine storm in fatal 2009 H1N1 cases
Aug 16, 2013
Researchers who studied lung tissue samples from 50 people who died of pandemic H1N1 (pH1N1) influenza infections in 2009 say they found clear evidence that the intense immune response known as a cytokine storm played a role in their demise.
The scientists found that the peak levels of virus in the victims' lungs correlated with "remarkably" high levels of certain cytokines in the same tissues, according to their report, which was released ahead of print this week in the American Journal of Pathology.
The abstract to the study is available at:
Cytokine and Chemokine Profiles in Lung Tissues from Fatal Cases of 2009 Pandemic Influenza A (H1N1
Role of the Host Immune Response in Pathogenesis
Rongbao Gao, Julu Bhatnagar, Dianna Blau, Patricia Greer, Dominique C. Rollin, Amy M. Denison, Marlene Deleon-Carnes, Wun-Ju Shieh, Suryaprakash Sambhara, Terrence M. Tumpey, Mitesh Patel, Lindy Liu, Christopher Paddock, Clifton Drew, Yuelong Shu, Jacqueline M. Katz, Sherif R. Zaki
While influenza can strike people of any age, it generally exacts its greatest toll on the elderly – those over the age of 65 - whose weaker immune systems (and comorbidities) can render them less able to fight off an infection.
Exact numbers are unknown, since influenza is only rarely cited as the primary cause of death. If a cause of death (beyond`natural causes’) is given, comorbidities like COPD, heart disease, asthma are far more likely to listed on a death certificate.
Still, estimates are that 90% of seasonal flu mortality occurs in those over the age of 65 (cite CDC Pink book).
In 2010, (see Study: Years Of Life Lost Due To 2009 Pandemic), researchers estimated the median age of death due to seasonal influenza-related illness in the United States to be 76.
In contrast, pandemic influenza strains, at least during the first few years after their introduction, often produce a dramatic `age shift’ downward in mortality.
The CDC’s estimate of average and median age of death due to the 2009 Pandemic virus reads:
Based on two CDC investigations of confirmed 2009 H1N1-related deaths that occurred during the spring and fall of 2009, the average age of people in the U.S. who died from 2009 H1N1 from April to July of 2009 was 40. The median age of death for this time period was 43. From September to October of 2009, the average age of people in the U.S. who died from 2009 H1N1 was 41, and the median age was 45.
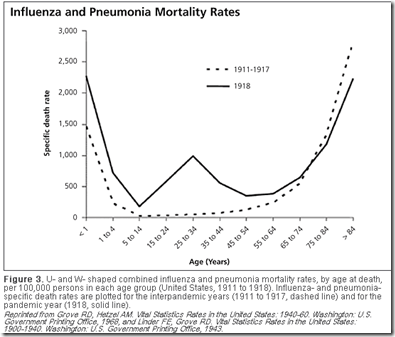
An even more pronounced `age shift’ was observed during the 1918 Spanish Flu, which exacted its heaviest toll among those aged 25 to 34 – an age group that would normally be expected to weather the illness better than any other.
The infamous `W shaped curve’ of the 1918 pandemic clearly shows that the death rates among those in their teens, 20s, and 30s was much higher than was normally seen in previous influenza years. Those over the age of 65, however, saw a reduction in mortality during the pandemic.
Similarly, the H5N1 avian flu virus has shown a disturbing predilection for younger victims, as illustrated by the following chart showing the ages of H5N1 cases in China over the past decade (see WHO Perspective Human infections with avian influenza A(H7N9) virus in China: preliminary assessments of the age and sex distribution).
.
Although not universally embraced, the Cytokine Storm theory has been adopted by many researchers as the most likely reason why the young, and healthy – those with presumably the most robust immune systems – would suffer disproportionately with some pandemic flu strains.
Somewhat surprisingly, we haven’t seen this age shift during the first wave of H7N9 avian flu cases in China this spring. We’ll have to see if this trend continues if, and when, the virus re-emerges.
As you can imagine, many researchers and doctors are looking for effective ways to safely dampen runaway immune responses as a possible treatment for pandemic influenza.
This is particularly important as most of the world would have little hope of seeing a vaccine for a pandemic flu during the first year or two of its arrival.
Dr. David Fedson – former Professor of Medicine at the University of Virginia School of Medicine and formerly Director of Medical Affairs, Aventis Pasteur MSD - has long championed the idea that we should be looking at statins for pandemic flu, which he believes may help modulate the immune response.
If they can be proved effective, statins have the advantage of being cheap, easy to manufacture and distribute, and have relatively few side effects.
The problem is, while some studies on statins and pneumonia have yielded promising results, not all of the research is in agreement. Complicating matters, since many statins are now generic, there is little financial incentive for drug companies to fund expensive research.
You can read about the potential for statin therapy in the blogs below.
Study: Statins, Influenza, & Mortality
Another Study On Statins And Pneumonia
There are other approaches under investigation as well.
In 2011, in Study: Calming The Cytokine Storm, we looked at research from The Scripps Research Institute that found a protein located on the surface of endothelial cells, called S1P1, to be largely responsible for flu-associated cytokine storms.
While a specific drug to target this protein is likely a long way off, their discovery provides new avenues for research into dampening the cytokine response.
This latest study in the American Journal of Pathology provides some of the strongest evidence we’ve seen on the impact of cytokine production in the pathogenesis of influenza.
Results that will likely spur additional interest in finding ways to moderate the cytokine storm.
For a better understanding of the pathogenesis of influenza, the innate immune system, and the role of cytokines I would invite you to read my 3-part look at the Baskin study from 2009.
Dissecting the Influenza Pathogenesis Study Pt. 1